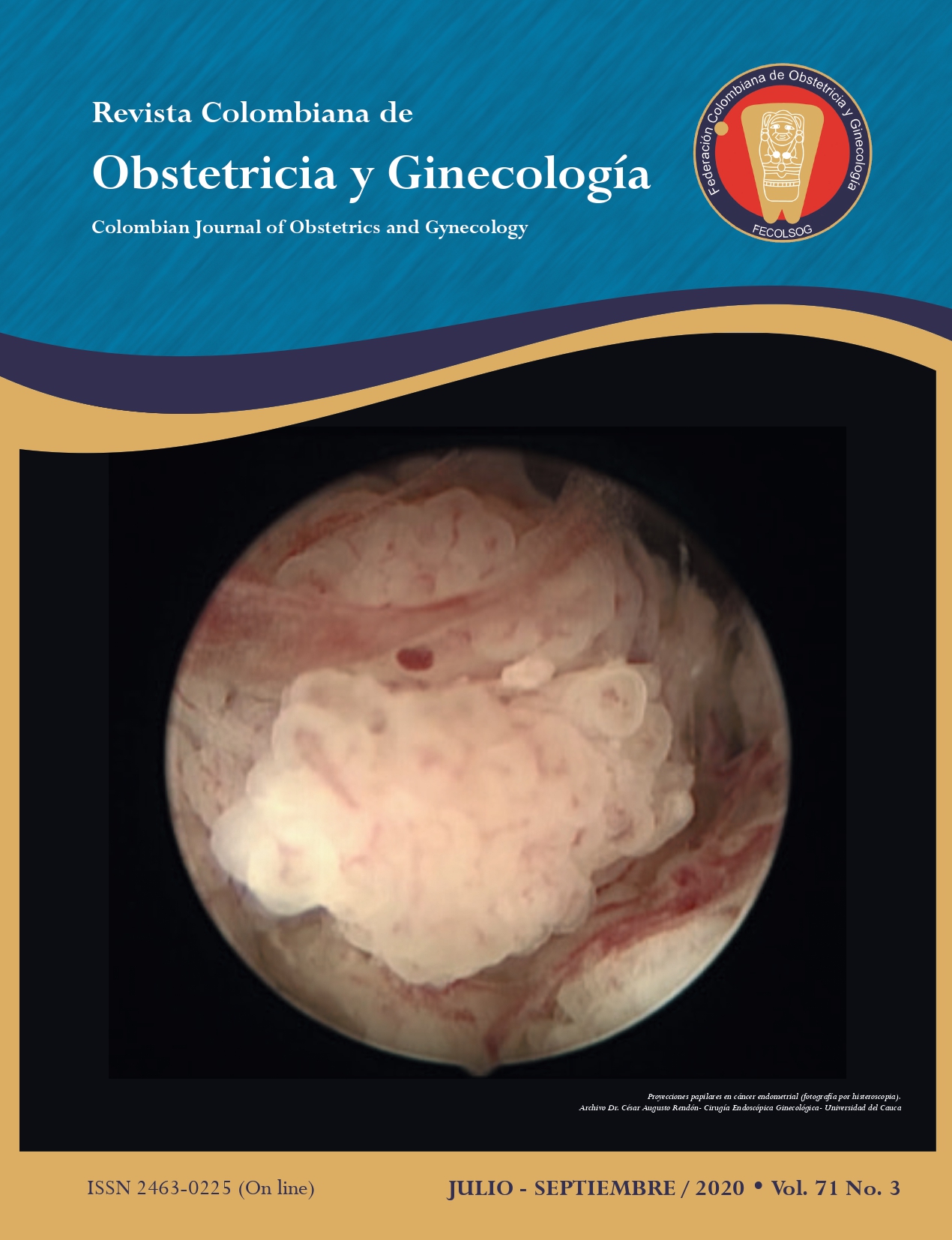
Diagnostic accuracy of a hysteroscopic score for the detection of endometrial cancer in patients with postmenopausal bleeding and endometrial thickening
DOI:
https://doi.org/10.18597/rcog.3445Abstract
Objective: To assess the diagnostic accuracy of hysteroscopic scores in endometrial cancer. Materials and methods: Diagnostic accuracy study assembled within a cross-sectional study that included patients with postmenopausal bleeding and endometrial thickening greater than 5 mm in whom hysteroscopy was performed and then compared with endometrial biopsy as the diagnostic gold standard, in two high complexity hospitals. Clinical, sociodemographic variables, as well as hysteroscopic scores and the results of endometrial tissue histopathology were measured. Sensitivity and specificity, likelihood ratios and area under the curve with their respective confidence intervals were estimated in the analysis. Results: With a 9% prevalence of endometrial cancer, the hysteroscopic assessment system was shown to have 75% sensitivity (95% CI; 30.1- 95.43), 95,1% specificity (95% CI; 83.9-98.7), a positive likelihood ratio of 15.38 (95%; CI 3.55- 66.56), a negative likelihood ratio of 0.26 and area under the curve of 85%. Conclusion: The standardized hysteroscopic assessment system was found to have an acceptable sensitivity for screening in patients with postmenopausal bleeding and endometrial thickening (≥ 5 mm). Further studies with larger sample sizes are required in order to arrive at a more precise estimation of the operational characteristics of the hysteroscopic assessment system for the detection of endometrial cancer.
Author Biographies
César Augusto Rendón-Becerra, Universidad del Cauca, Popayán (Colombia).
Médico cirujano, especialista ginecología y obstetricia; cirugía endoscópica ginecológica, Departamento de Ginecología y Obstetricia, Facultad Ciencias de la Salud, Universidad del Cauca, Popayán (Colombia).
Alex Gómez-Bravo, Universidad del Cauca, Popayán (Colombia).
Médico general, Facultad Ciencias de la Salud, Universidad del Cauca, Popayán (Colombia).
Andrés Felipe Erazo-Narváez, Universidad del Cauca, Popayán (Colombia).
Médico general, Facultad Ciencias de la Salud, Universidad del Cauca, Popayán (Colombia).
Roberth Alirio Ortiz-Martínez, Universidad del Cauca, Popayán (Colombia).
Médico cirujano, especialista ginecología y obstetricia; magíster en Epidemiología, Departamento de Ginecología y Obstetricia, Facultad Ciencias de la Salud, Universidad del Cauca, Popayán (Colombia).
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2015. CA Cancer J Clin. 2015;65(1):5-29. https://doi.org/10.3322/caac.21254
World Health Organization. International Agency for Research on Cancer. Global Cancer Observatory 2018. Disponible en: https://gco.iarc.fr/today/home
SGO Clinical Practice Endometrial Cancer Working Group, Burke WM, Orr J, Leitao M, Salom E, Gehrig P, et al. Endometrial cancer: A review and current management strategies: Part I. Gynecol Oncol. 2014;134(2):385-92. https://doi.org/10.1016/j.ygyno.2014.05.018
Body N, De Kerdaniel O, Lavoué V, Leblanc M, Henno S, Levêque J. Early-stage endometrial cancer: Sentinel node or lymphadenectomy? Gynecol Obstet Fertil. 2016;44(4):239-43. https://doi.org/10.1016/j.gyobfe.2016.02.015
Practice Bulletin No. 149: Endometrial cancer. Obstet Gynecol. 2015;125:1006-26. https://doi.org/10. 1097/01.AOG.0000462977.61229.de
Munro MG, Critchley HOD, Fraser IS, Haththotuwa R, Kriplani A, Bahamondes L, et al. The two FIGO systems for normal and abnormal uterine bleeding symptoms and classification of causes of abnormal uterine bleeding in the reproductive years: 2018 revisions. Int J Gynecol Obstet. 2018;143(3):393-408. https://doi.org/10.1002/ijgo.12666
American College of Obstetricians and Gynecologists. The role of transvaginal ultrasonography in evaluating the endometrium of women with postmenopausal bleeding. ACOG Committee Opinion No. 734. Obstet Gynecol. 2018;131(5):e124-9.
Wong A, Lao T, Cheung CW, Yeung SW, Fan HL, Ng PS, et al. Reappraisal of endometrial thickness for the detection of endometrial cancer in postmenopausal bleeding: A retrospective cohort study. BJOG. 2016;123(3):439-46. https://doi.org/10.1111/1471-0528.13342
da Cunha-Vieira M, Costa-Rossette M, Cavalcanti L. Histeroscopia y cáncer endometrial. En: Cirugía Mínimamente Invasiva en Ginecología; Bogotá: Federación Latinoamericana de Sociedades de Obstetricia y Ginecología (FLASOG). AltaVoz Editores; 2017. p. 482-6.
Ghoubara A, Emovon E, Sundar S, Ewies A. Thickened endometrium in asymptomatic postmenopausal women–determining an optimum threshold for prediction of atypical hyperplasia and cancer. J Obstet Gynaecol (Lahore). 2018;38(8):1146-9. https://doi.org/10.1080/01443615.2018.1458081
Clark TJ, Voit D, Gupta JK, Hyde C, Song F, Khan KS. Accuracy of hysteroscopy in the diagnosis of endometrial cancer and hyperplasia. A systematic quantitative review. JAMA. 2002;288(13):1610-21. https://doi.org/10.1001/jama.288.13.1610
Miyamoto T, Abiko K, Murakami R, Furutake Y, Baba T. Hysteroscopic morphological pattern reflects histological grade of endometrial cancer. J Obstet Gynaecol Res. 2019;45(8):1-9. https://doi.org/10.1111/jog.13998
Dueholm M, Hjorth IMD, Secher P, Jørgensen A, Ørtoft G. Structured hysteroscopic evaluation of endometrium in women with postmenopausal bleeding. J Minim Invasive Gynecol. 2015;22(7):1215-24. https://doi.org/10.1016/j.jmig.2015.06.018
Clarke MA, Long BJ, Morillo ADM, Arbyn M, Bakkum-Gamez JN, Wentzensen N. Association of endometrial cancer risk with postmenopausal bleeding in women a systematic review and meta-analysis. JAMA Intern Med. 2018;178(9):1210-22. https://doi.org/10.1001/jamainternmed.2018.2820
Weiderpass E, Antoine J, Bray FI, Oh J-K, Arbyn M. Trends in corpus uteri cancer mortality in member states of the European Union. Eur J Cancer. 2014;50(9):1675-84. https://doi.org/10.1016/j.ejca.2014.02.020
Leeflang MM, Bossuyt PM, Irwig L. Diagnostic test accuracy may var y with prevalence: Implications for evidence-based diagnosis. J Clin Epidemiol. 2009;62(1):5-12. https://doi.org/10.1016/j.jclinepi.2008.04.007
Habibzadeh F, Habibzadeh P, Yadollahie M. On determining the most appropriate test cut-off value: The case of tests with continuous results. Biochem Med (Zagreb). 2016;26(3):297-307. https://doi.org/10.11613/BM.2016.034
Amant F, Raza M, Koskas M, Creutzberg C. Cancer of the corpus uteri. J Obstet Gynaecol (Lahore). 2018;143(2):37-50. https://doi.org/10.1002/ijgo.12612
World Medical Association. Declaration of Helsinki. Ethical principles for medical research involving human subjects. J Am Med Assoc. 2015;310(20):2013-6. https://doi.org/10.1001/jama.2013.281053
Ministerio de Salud y Protección Social. Resolución 8430, Por la cual se establecen las normas científicas, técnicas y administrativas para la investigación en salud. Bogotá: Ministerio de Salud; 1993 Disponible en: https://www.minsalud.gov.co/sites/rid/Lists/BibliotecaDigital/RIDE/DE/DIJ/RESOLUCION-8430-DE-1993.PDF
Gkrozou F, Dimakopoulos G, Vrekoussis T, Lavasidis L, Koutlas A, Navrozoglou I, et al. Hysteroscopy in women with abnormal uterine bleeding: A metaanalysis on four major endometrial pathologies. Arch Gynecol Obs. 2015;291(6):1347-54. https://doi.org/10.1007/s00404-014-3585-x
Lasmar RB, Barrozo PR, de Oliveira MA, Coutinho ES, Dias R. Validation of hysteroscopic view in cases of endometrial hyperplasia and cancer in patients with abnormal uterine bleeding. J Minim Invasive Gynecol. 2006;13(5):409-12. https://doi.org/10.1016/j.jmig.2006.05.002
How to Cite
Downloads
Downloads
Published
Issue
Section
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |