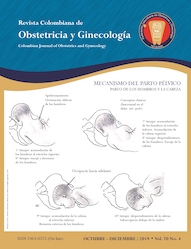
Breech presentation delivery care: A review of childbirth semiology, mechanism and care
DOI:
https://doi.org/10.18597/rcog.3345Keywords:
Breech presentation, obstetric complications of childbirth, continuing medical education, dystociaAbstract
Objective: To review the concepts underlying breech presentation delivery as well as the semiology and the obstetric maneuvers contributing to a successful perinatal maternal outcome.
Materials and methods: Based on a hypothetical scenario to set the stage for a practical approach to the topic, an explanatory paper built on a narrative review is created in order to examine the principles related to diagnosis, mechanism of delivery and maternal care, emphasizing maneuvers to ease fetal extraction.
Results: Breech presentation delivery must be managed through the vaginal canal when already in the expulsion phase with fetal engagement. For diagnosis and care, it is essential to know the unique semiology and physiology of this condition as well as the obstetric maneuvers to facilitate an uncomplicated delivery.
Conclusions: The mechanism of childbirth in breech presentation is complex and requires knowledge of its physiology and multiple obstetric maneuvers on the part of the obstetrician as well as the general practitioner, in order to ensure adequate care when there is no other option.
Author Biographies
Carlos Fernando Grillo-Ardila, Universidad Nacional de Colombia
Profesor asistente: docente de cátedra, Departamento de Obstetricia y Ginecología, Universidad Nacional de Colombia.
Alejandro Antonio Bautista-Charry, Universidad Nacional de Colombia
Profesor Asociado; director del Departamento de Obstetricia y Ginecología, Universidad Nacional de Colombia.
Mariana Diosa-Restrepo, Universidad Nacional de Colombia
Residente de tercer año de Obstetricia y Ginecología, Facultad de Medicina, Universidad Nacional de Colombia.
References
The Royal Women`s Hospital, Victoria Australia. Management of breech presentation, Clinical Guideline. 2012. Disponible en: https://www.thewomens.org.au/health-professionals/clinicalresources/clinical-guidelines-gps/ .
Ñáñez H, Ruiz A, Ángel E, Bautista A, Sabogal J. Distocias. En: Ñáñez H, Ruiz A (eds.). Texto de obstetricia y perinatología. Bogotá: Lito Camargo; 1999. p. 105-121.
Botella-Llusia J, Clavero-Núnez J. Distocias de los elementos del parto. Presentación podálica. Clasificación y nomenclatura. En: Tratado de ginecología, Tomo II, Patología obstétrica. 12 ed. Barcelona, Editorial Científica Médica; 1981. p. 575-599.
Arias F, editor. Abnormal Labor and delivery. En: Practical Guide to High-risk Pregnancy. 2 ed. Mosby Year Book; 1993. p. 402.
Royal College of Obstetricians & Gynaecologists. Management of Breech Presentation, Clinical Guideline. UK 2017. Disponible en: https://www.rcog.org.uk/en/guidelines-research-services/guidelines/gtg20b/.
The Royal Australian and New Zealand College of Obstetricians and Gynecologists. Management of Breech Presentation at Term, Clinical Guideline. 2016. Disponible en: https://www.ranzcog.edu.au/RANZCOG_SITE/media/RANZCOG-MEDIA/Women%27s%20Health/Statement%20and%20guidelines/Clinical-Obstetrics/Management-of-breech-presentation-at-term-(CObs-11)-Review-July-2016pdfBreechPresentation-InTheAntenatalPeriodAndBreechDeliveryClinical-GuidelinesForTheManagementOf.pdf.
Royal Cornwall Hospital. Clinical Guideline for the Management of a Breech Presentation in the Ante Natal Period, External Cephalic Version (ECV) and Breech Presentation in Labour, UK 20212. Disponible en: http://www.rcht.nhs.uk/DocumentsLibrary/RoyalCornwallHospitalsTrust/Clinical/MidwiferyAndObstetricsBreechPresentationInTheAntenatalPeriodAndBreechDeliveryClinical-GuidelinesForTheManagementOf.pdf.
Fianu S, Václavínková V. The site of placental attachment as a factor in the aetiology of breech presentation. Acta Obstet Gynecol Scand. 1978;57(4):371-2. https://doi.org/10.3109/00016347809154033
Cabero-Roura L. Patología del parto (III): Presentaciones anormales. El parto de nalgas. Conducta obstétrica. En: Cabero-Roura L, Saldivar-Rodríguez D, Cabrill-Rodríguez E. Obstetricia y medicina Maternofetal. Madrid: Editorial Médica Panamericana; 2007. p. 994.
Duffy CR, Moore JL, Saleem S, Tshefu A, Bose CL, Chomba E, et al. Malpresentation in low- and middleincome countries: Associations with perinatal and maternal outcomes in the Global Network. Acta Obstet Gynecol Scand. 2019; 98(3):300-8. https://doi.org/10.1111/aogs.13502.
Kozuki N, Katz J, Khatry SK, Tielsch JM, LeClerq SC, Mullany LC. Risk and burden of adverse intrapartumrelated outcomes associated with non-cephalic and multiple birth in rural Nepal: A prospective cohort study. BMJ Open. 2017;7(4):e013099. http://dx.doi.org/10.1136/bmjopen-2016-013099
Dohbit JS, Foumane P, Tochie JN, Mamoudou F, Temgoua MN, Tankeu R, et al. Maternal and neonatal outcomes of vaginal breech delivery for singleton term pregnancies in a carefully selected Cameroonian population: A cohort study. BMJ Open. 2017;7(11):e017198. https://doi.org/10.1136/bmjopen-2017-017198.
Fonseca A, Silva R, Rato I, Neves AR, Peixoto C, Ferraz Z, et al. Breech presentation: Vaginal versus cesarean delivery, which intervention leads to the best outcomes? Acta Med Port. 2017;30(6):479-84. https://doi.org/10.20344/amp.7920.
Lai S, Flatley C, Kumar S. Perinatal risk factors for low and moderate Five-minute Apgar scores at term. Eur J Obstet Gynecol Reprod Biol. 2017;210:251-6. https://doi.org/10.1016/j.ejogrb.2017.01.008.
Mid Essex Hospital Ser vices. Management of breech birth 4.0. UK 2014. (Visitado 2018, dic 29). Disponible en: http://www.meht.nhs.uk/search/?q=breech.
Yeoh SGJ, Rolnik DL, Regan JA, Lee PYA. Experience and confidence in vaginal breech and twin deliveries among obstetric trainees and new specialists in Australia and New Zealand. Aust N Z J Obstet Gynaecol. 2019;59(4):545-9. https://doi.org/10.1111/ajo.12931.
Petrovska K, Sheehan A, Homer CSE. The fact and the fiction: A prospective study of internet forum discussions on vaginal breech birth. Women Birth. 2017;30(2):e96-e102. https://doi.org/10.1016/j.wombi.2016.09.012.
Interim Update ACOG Committee Opinion No. 745. American College of Obstetricians and Gynecologists. Mode of term singleton breech deliver y. Obstet Gynecol. 2018;e60-E63. https://doi.org/10.1097/AOG.0000000000002755
Hofmeyr GJ, Kulier R. External cephalic version for breech presentation atterm. Cochrane Database Syst Rev. 2012;10:CD000083. https://doi.org/10.1002/14651858.CD000083.pub2.
Auckland District Health Board, National Women`s Hospital, Auckland New Zealand. Breech birth. Clinical Guideline. 2012. Disponible en: http://nationalwomenshealth.adhb.govt.nz/healthprofessionals/policies-and-guidelines
Nottingham University Hospital. Guideline for the management of singleton breech presentation in pregnancy and labour. UK 2012. Disponible en: https://www.nuh.nhs.uk/download.cfm?doc=docm93jijm4n1050.pdf&ver=11159
East Cheshire Hospital. Breech presentation. Clinical Guideline. UK 2013. Disponible en: http://www.eastcheshire.nhs.uk/About-TheTrust/policies/M/Maternity%20Breech%20Presentation%201907.pdf
León J. El parto en presentación pelviana. En: Tratado de Obstetricia. Tomo I. Buenos Aires: Editorial Científica Argentina; 1956. p. 1066-1115.
Peralta Cayón R. Presentación de pelvis y de hombros. En: Obstetricia y Clínica Obstétrica. Bogotá: Imprenta Antares; 1956. P. 697-753.
Kotaska A, Menticoglou S, Gagnon R. Maternal Fetal Medicine Committee. Vaginal deliver y of breech presentation. J Obstet Gynaecol Can. 2009;31(6):557-66. https://doi.org/10.1016/S1701-2163(16)34221-9
Louwen F, Daviss BA, Johnson KC, Reitter A. Does breech delivery in an upright position instead of on the back improve outcomes and avoid cesareans? Int J Gynaecol Obstet. 2017;136(2):151-61. https://doi.org/10.1002/ijgo.12033.
Rabe H, Diaz-Rossello JL, Duley L, Dowswell T. Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database of Systematic Reviews. 2012; Issue 8. Art. CD003248. https://doi.org/10.1002/14651858.CD003248.pub3.
Currea-Guerrero S. La adaptación neonatal inmediata: la reanimación neonatal. Bogotá: Universidad Nacional de Colombia; 2004.
Muñoz-Arbat J. Extracción manual del feto y versión. En: Nubiola P, Zárate E, editores. Tratado de Obstetricia. Barcelona: Editorial Labor; 1951. p. 963-1020.
Lee J, Greenhill JP, Carrera O, Peralta A, Carrasco R. Anormalidades por parte del feto presentación de nalgas. En: Principios y práctica de obstetricia. Tomo II. México: Unión Tipográfica - Editorial Hispano Americana; 1947. p. 790-830.
Dexus Trias de Bes S, Carrera Macia JM. Parto podálico operatorio. En: Tratado de Obstetricia Dexeus. Volumen III: Tratado y atlas de Operatoria Obstétrica. 2 ed. Barcelona: Salvat Editores; 1988.
Schwarcz RL, Duverges CA, Diaz G, Fescina RH. Obstetricia. El parto en las distintas presentaciones. 5 ed. Buenos Aires: El Ateneo; 1997. p. 450.
UMVF – Université Médicale Virtuelle Francophone. Manoeuvres obstétricales. Comité éditorial de l’UVMaF 2013-2014. p. 4-29.
Feliz Báez CA. Presentación pélvica. Manual de maniobras y procedimientos en Obstetricia. Bogotá: McGraw-Hill; 2005. p. 235-245.
Dunn PM. Erich Bracht (1882-1969) of Berlin and his “breech” manoeuvre. Arch Dis Child Fetal Neonatal Ed. 2003;88(1):F76-7. https://doi.org/10.1136/fn.88.1.f76
Lovset J. Shoulder delivery by breech presentation. J Obstete Gynaecol. 1973;44:696-704. https://doi.org/10.1111/j.1471-0528.1937.tb14687.x
Pschyrembel W. Presentación de la extremidad pélvica. En: Obstetricia práctica. 3 ed. Buenos Aires: Editorial Labor; 1978. p. 135-164.
How to Cite
Downloads
Downloads
Published
Issue
Section
License
Copyright (c) 2020 Revista Colombiana de Obstetricia y Ginecología

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
| Article metrics | |
|---|---|
| Abstract views | |
| Galley vies | |
| PDF Views | |
| HTML views | |
| Other views | |